Le glaucome est une maladie chronique et irréversible qui détruit progressivement les fibres nerveuses du nerf optique entraînant une atteinte du champ visuel. Dans la plupart des cas, le champ visuel commence à se dégrader dans la zone périphérique, ce qui cause la «vue en tunnel».
Il peut être dû à plusieurs causes, le facteur de risque le plus important étant l’élévation de la pression oculaire.
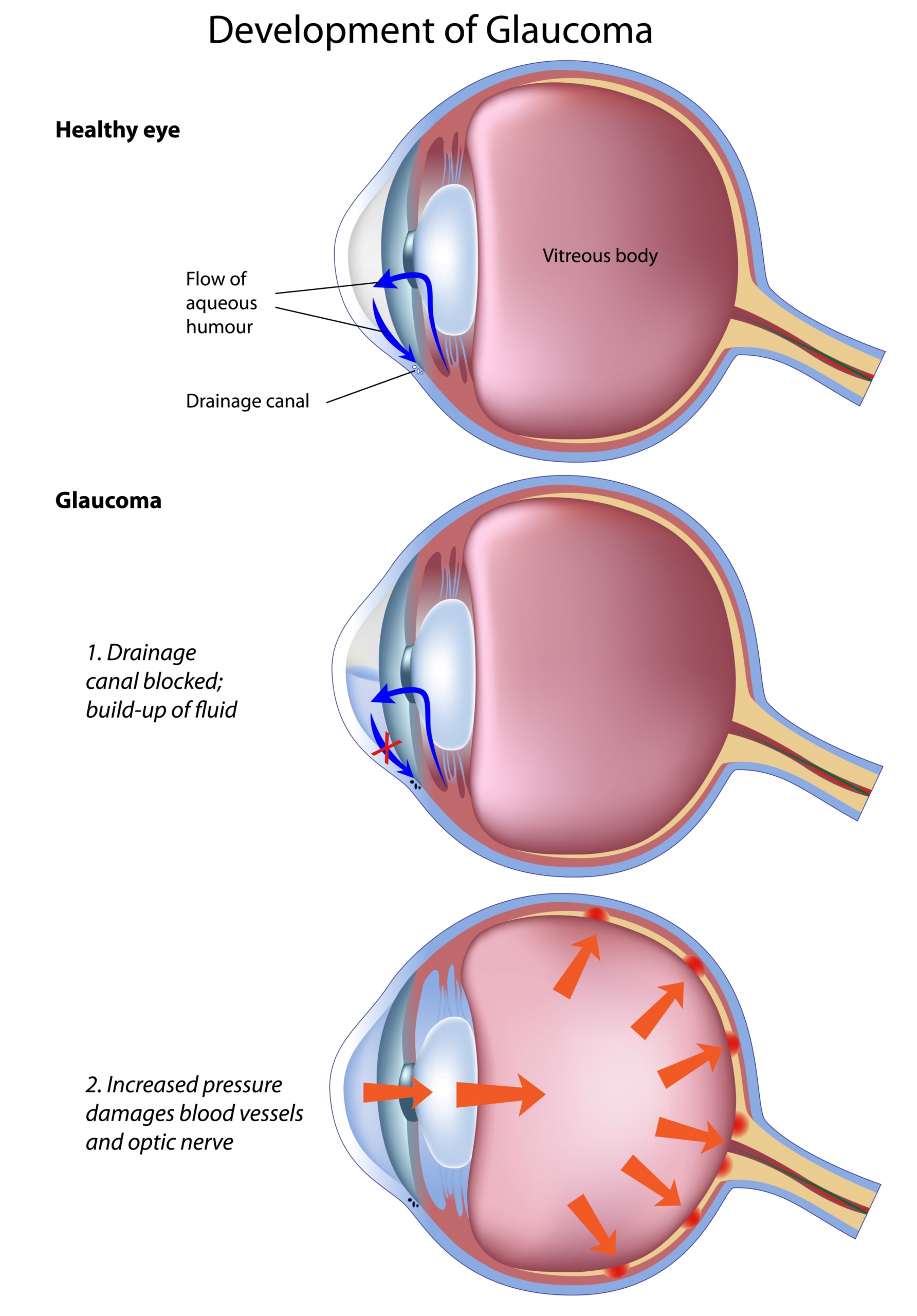
La pression intraoculaire résulte de la vitesse de production de l’humeur aqueuse (liquide transparent qui permet de maintenir la forme de l’œil) et par la résistance à son écoulement.
Il existe différentes formes de glaucome, classées selon leur physiopathologie.
On distingue notamment entre glaucome primaire et secondaire ainsi qu’entre glaucome à angle ouvert et à angle fermé. La majorité (>90%) des patients présentent un glaucome primaire à angle ouvert qui touche environ 2 % de la population de plus de 40 ans et constitue une des causes principales de cécité dans le monde.
Glaucome et pression intraoculaire
Une pression intraoculaire augmentée n’aboutit pas toujours à un glaucome car la susceptibilité de chaque nerf optique varie pour chaque personne. On parle d’hypertension oculaire lorsque l’œil présente une pression intraoculaire élevée sans lésion du nerf optique. Seul l’ophtalmologue peut savoir si la tension oculaire doit être traitée ou pas. Même si un traitement n’est pas (encore) nécessaire, il faudra cependant réaliser des contrôles réguliers.
À l’opposé, ce n’est pas parce que la mesure d’une pression intraoculaire est normale qu’il n’y a pas de glaucome. Certaines personnes ont un nerf optique tellement vulnérable qu’elles développent des dégâts glaucomateux avec une pression oculaire dans les limites statistiques de la normale (on parle de « glaucome à pression normale »). Seul l’ophtalmologue peut détecter des changements du nerf optique, ordonner les examens adéquats et instaurer un traitement.
Symptômes
Le glaucome est une maladie sournoise ; le patient ne s’aperçoit de dégâts visuels liés au glaucome que dans un stade très avancé.
Seul l’ophtalmologue est capable de dépister les premiers signes en examinant le nerf optique et en demandant la réalisation d’examens supplémentaires comme par exemple un champ visuel.
Étant donné que l’atteinte du nerf optique est irréversible, il ne faut donc pas hésiter pour demander un dépistage.
Symptômes
Le glaucome est une maladie sournoise ; le patient ne s’aperçoit de dégâts visuels liés au glaucome que dans un stade très avancé.
Seul l’ophtalmologue est capable de dépister les premiers signes en examinant le nerf optique et en demandant la réalisation d’examens supplémentaires comme par exemple un champ visuel.
Étant donné que l’atteinte du nerf optique est irréversible, il ne faut donc pas hésiter pour demander un dépistage.
Facteurs de risque
antécédents familiaux de glaucome
âge : l’incidence du glaucome augmente à partir de 40 ans
sujet mélanoderme
prise de corticoïdes (ancienne ou récente)
hypertension artérielle et maladies cardiovasculaires
hypotension artérielle (iatrogène, nocturne ou orthostatique)
diabète sucré
myopie forte
vasospasmes (syndrome de Raynaud, migraine)
Méthodes d’examen
fond de l’œil : examination du nerf optique et de son excavation
mesure de la pression intraoculaire : en moyenne de 15 mmHg chez l’adulte
champ visuel/périmétrie : met en évidence des atteintes glaucomateuses précoces
OCT de la papille : mesure l’épaisseur des fibres optiques
HRT : mesure la taille et la profondeur de l’excavation papillaire.
gonioscopie : examen de l’angle de la chambre antérieure pour déterminer le type de glaucome
pachymétrie : examen de l’épaisseur de la cornée pour apprécier la pression mesurée
Traitement
Le traitement a pour objectif de stabiliser la maladie afin de préserver la fonction visuelle. Le but est d’abaisser la pression intraoculaire. En général les collyres hypotonisants sont proposés en première intention, mais les traitements laser ou une chirurgie peuvent être indiqués dès le début.Le glaucome est aujourd’hui contrôlable dans la plupart des cas, à condition de réaliser des contrôles réguliers et de suivre les instructions de son ophtalmologue.
Traitement médical : il repose en général sur l’instillation de gouttes dans les yeux. La prise d’un médicament par voie générale est beaucoup plus rare.
Les collyres hypotonisants oculaires sont nombreux ; ils agissent par diminution de la production d’humeur aqueuse ou par augmentation de son évacuation.
Laser : il existe différents types de laser adaptés à différents types de glaucome.
Chirurgie : en général une chirurgie n’est nécessaire que si la maladie progresse malgré un traitement médical ou après un traitement par laser. Il existe plusieurs techniques chirurgicales.
Prévention
La précocité du diagnostic est essentielle et du domaine de l’ophtalmologue. Au plus tard vers 40 ans un contrôle régulier de la pression intraoculaire s’impose chez toutes les personnes.Une fois le diagnostic posé, il est important d’appliquer le collyre de manière régulière, sans interruption et de respecter les contrôles fixés avec l’ophtalmologue.
Nous prenons en charge l’ensemble des maladies de l’œil,
du diagnostic initial au suivi régulier.